Earlier this year, when we went into lockdown, some of our staff with expertise in palliative care were redeployed to help others. They were re-deployed to help adults in Oxfordshire, who had been diagnosed with COVID-19, at both Katharine House Hospice in Banbury and at Oxford University Hospitals NHS Foundation Trust, which was under the direction of Sobell House. The main benefit of this collaborative working was the pooling of expertise to ensure the best patient care could be delivered to COVID-19 patients in Oxfordshire, where there was an increased demand.
As a children’s hospice, we are part of the Oxfordshire Palliative Care network and have been working together to share knowledge and experience with other members for some time now. However, this instance was unique as it was the first time we had worked together directly caring for patients. It was very clear that, with the outbreak of COVID-19 in Oxfordshire, there would be stresses and strains on resources to cope with patient care, so resources needed to be redistributed amongst the nursing and medical teams.
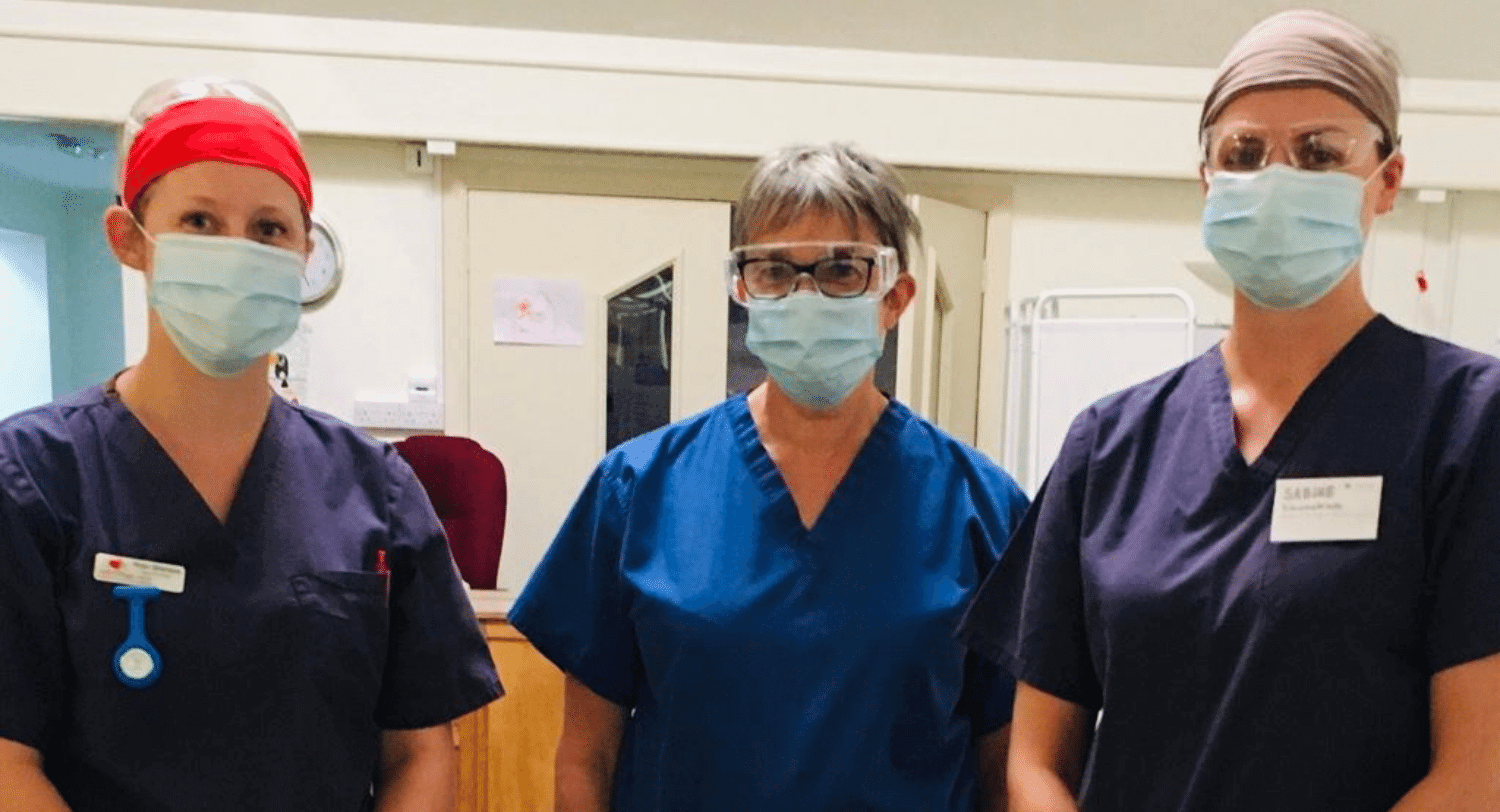
Children, even those with life-shortening conditions, are thankfully not as badly affected by COVID-19 as some vulnerable adults are, which inevitably freed up some of our resources at Helen & Douglas House and meant we were able to help other healthcare providers in the region. Whilst vital stays for symptom management and end-of-life care has continued to be delivered at the hospice, the remainder of the care we were able to provide was mainly limited to help them at home through regular visits, phone and video calls and emails. At the start of lockdown, all previously booked respite stays were cancelled, as most of our families chose to shield to keep their children away from the virus, which meant we had the capacity to help.
So in early April, the request came in for Helen & Douglas House staff to be seconded to Katharine House, which was a COVID-19 Response Centre and had subsequentially increased its beds. Arrangements took around a week to put in place and we saw three of our nurses, and two of our nursery nurses, move over to the adult hospice around Easter time. These arrangements then remained in place for 16 weeks.
Dr Emily Harrop, Consultant in Paediatric Palliative Care & Medical Director at Helen & Douglas House, also helped the adult palliative care team by supporting patients on the re-commissioned surgical wards at the John Radcliffe Hospital and at Sobell House. She explained a bit more about why collaborative working was so important, especially at this time.
‘Nurses and junior doctors, who normally work in acute general medicine or general surgery at the John Radcliffe Hospital, were having to give palliative care to more patients for the first time. This was a massive change in the type of clinical care they were used to delivering, so worked together to share our experience in palliative care and allowed space for informal debriefs to help them. Although this is new to many of these nurses and junior doctors, they are doing were, and are, doing a more amazing job than they realise because of their extraordinary levels of compassion.
‘As well as this, all of us are adapting to a new way of working as it is very different giving palliative care with PPE and face masks on, especially when communicating with patients at the end of their lives. It is very difficult because they cannot see your facial expressions and compassion and holding their hand with gloves on is just not the same.
‘A palliative care ward is very different from a normal surgical ward, where you are usually rushing about, providing a much more acute type of care to patients who are recovering from operations. On palliative care wards more time is spent with each patient.
‘It has also been very different and challenging for our nurses working at Katharine House Hospice. They have experienced a higher turnover of patients, with most only staying for short periods of time, a type of nursing care which is quite different to the palliative care we deliver at a children’s hospice. Despite this, we were overwhelmed by the positive response from our nursing team who volunteered to do this.
‘As a result of this collaborative and flexible way of working, all parties have gained; the patients have had the best patient care and the staff have learnt new skills, so it has been a great experience which has benefited everyone.’
Our staff members who were redeployed are have recently come back to Helen & Douglas House and it is great to see them back in-house caring for our children and families again.
We have now welcomed these members of the care team back from their secondment. Your continued support means we have been able to continue to care for local terminally ill children throughout this pandemic, at the hospice, with symptom management and end of life care, as well as at home. Since the pandemic started in March, your donations have helped fund end of life care and support to a number of children that we care for and has meant we have been able to be their families who continue to need our help. Local terminally ill children and their families need your help today so please make a donation to Helen & Douglas House.